Impact Factor ISSN: 1449-1907
Int J Med Sci 2022; 19(11):1706-1714. doi:10.7150/ijms.75835 This issue Cite
Research Paper
A comparison between bronchial blockers and double-lumen tubes for patients undergoing lung resection: A propensity score-matched cohort study
1. Department of Anesthesiology, The Second Xiangya Hospital, Central South University, Changsha, Hunan Province, China.
2. Department of Thoracic Surgery, The Second Xiangya Hospital, Central South University, Changsha, Hunan Province, China.
*These authors contributed equally to this work.
Abstract
Objective: The aim of this study is to compare the effect of bronchial blockers (BB) and double-lumen tubes (DLT) on patients' postoperative recovery after lung resection.
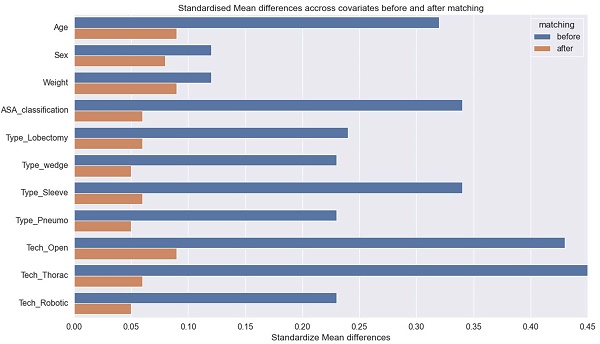
Method: 4,636 patients undergoing lung resection and receiving either BB or DLT intubation were reviewed and matched using the propensity score matching method. The primary outcome was the surgical duration. The secondary outcomes included diagnostic results of postoperative chest X-ray, postoperative oxygenation index, incidence of hypercapnia, hypoxemia and sore throat, chest tube duration, incidence of ICU admission, length of hospital stay and incidence of the 30-day readmission.
Results: After matching, 401 patients receiving BB were matched to 3,439 patients receiving DLT. There was no statistical difference on the surgical duration between the two groups (P>0.05). However, compared with the DLT group, patients in the BB group showed more infiltrate especially at the surgery side (14.96% versus 9.07%, P<0.001) based on the chest X-ray, together with higher incidence of ICU admission (5.23% versus 2.61%, P<0.05). Additionally, no statistical differences were found between the two groups about chest tube duration, oxygenation index, incidence of hypercapnia, hypoxemia and sore throat, duration of surgery, hospital stays and 30-day readmission (P>0.05).
Conclusions: Compared with the DLT, patients receiving BB technique tend to have increased pulmonary infiltrate (especially the surgery side) and higher incidence of ICU admission at the early post-operative stage, which may have an influence on the patients' recovery.
Keywords: bronchial blocker (BB), double-lumen tube (DLT), one-lung ventilation (OLV), lung resection, postoperative recovery, postoperative morbidity, propensity score matching, retrospective study

 Global reach, higher impact
Global reach, higher impact