3.2
Impact Factor
ISSN: 1449-1907
Int J Med Sci 2021; 18(14):3280-3289. doi:10.7150/ijms.62010 This issue Cite
Research Paper
Association of Hepatic Steatosis Index and Fatty Liver Index with Carotid Atherosclerosis in Type 2 Diabetes
1. Department of Endocrinology, Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu 212001, China
2. Department of Nephrology, Affiliated Hospital of Jiangsu University, Zhenjiang, Jiangsu 212001, China
*These authors contributed equally to this work.
Abstract
Background/aim: Previous studies have suggested that the hepatic steatosis index (HSI) and fatty liver index (FLI) can be used as a predictor of non-alcoholic fatty liver disease (NAFLD). The aim of our study was to determine whether non-invasive indices of hepatic steatosis (HSI and FLI) are associated with carotid atherosclerosis in type 2 diabetes mellitus (T2DM).
Methods: This was a cross-sectional study conducted in the T2DM patients (n=768). Carotid intima-media thickness (CIMT) was measured by the Color Doppler ultrasound. The HSI was calculated based on gender, body mass index (BMI), and transaminases level. The FLI was based on BMI, waist circumference (WC), triacylglycerols (TG) and g-glutamyl transferase (GGT).
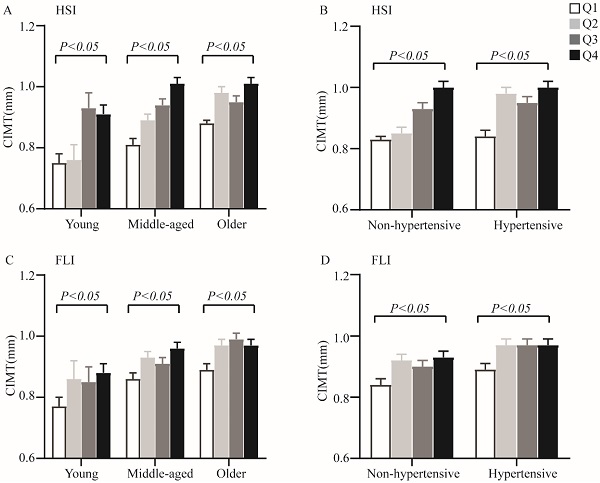
Results: Raised HSI and FLI levels was associated with increased CIMT levels in T2DM patients. Patients with greater CIMT had higher HSI (39.10 ± 5.70 vs 36.10 ± 4.18, P < 0.001) and FLI (46.35 (29.96, 65.54) vs 36.93 (18.7, 57.93), P < 0.001) than those with lower CIMT. Subjects with existing carotid plaque had higher HSI (38.28 ± 5.63 vs 35.69 ± 3.45 P < 0.001) and FLI (47.41 (27.77, 66.62) vs 37.19 (17.71, 51.78), P < 0.001) accordingly. HSI (r = 0.343, P < 0.001) and FLI (r = 0.184, P < 0.001) were positively related with the CIMT. In the linear regression, after full adjustment metabolic risk factors, smoking, and measures of insulin resistance, HSI and FLI were independently associated with CIMT (HSI: β = 0.011, FLI: β = 0.001, all P < 0.01). Further, logistic regression analyses showed that higher HSI and FLI had an impact on the risk for carotid atherosclerosis [HSI: OR (95%CI): 1.174 (1.123-1.228), FLI: OR (95%CI): 1.011(1.004-1.019), all P < 0.01]. Overall, increasing values of HSI and FLI were associated with CIMT (P < 0.05) significantly across different categories of age and hypertension.
Conclusion: Current data suggest HSI and FLI are independently correlated with carotid atherosclerosis in T2DM. They may be a simple and useful marker for assessing the progression of diabetic macrovascular complications.
Keywords: Hepatic steatosis index, Fatty liver index, Type 2 diabetes, Carotid atherosclerosis, Macrovascular complication

 Global reach, higher impact
Global reach, higher impact