Impact Factor
ISSN: 1449-1907
Int J Med Sci 2021; 18(8):1739-1745. doi:10.7150/ijms.51235 This issue Cite
Research Paper
Machining learning predicts the need for escalated care and mortality in COVID-19 patients from clinical variables
1. Department of Family, Population and Preventive Medicine, Renaissance School of Medicine at Stony Brook University, Stony Brook, New York, United States of America.
2. Department of Radiology, Renaissance School of Medicine at Stony Brook University, Stony Brook, New York, United States of America.
3. Department of Radiology, Montefiore Medical Center and Albert Einstein College of Medicine, Bronx, New York, United States of America.
Abstract
Objective: This study aimed to develop a machine learning algorithm to identify key clinical measures to triage patients more effectively to general admission versus intensive care unit (ICU) admission and to predict mortality in COVID-19 pandemic.
Materials and methods: This retrospective study consisted of 1874 persons-under-investigation for COVID-19 between February 7, 2020, and May 27, 2020 at Stony Brook University Hospital, New York. Two primary outcomes were ICU admission and mortality compared to COVID-19 positive patients in general hospital admission. Demographic, vitals, symptoms, imaging findings, comorbidities, and laboratory tests at presentation were collected. Predictions of mortality and ICU admission were made using machine learning with 80% training and 20% testing. Performance was evaluated using receiver operating characteristic (ROC) area under the curve (AUC).
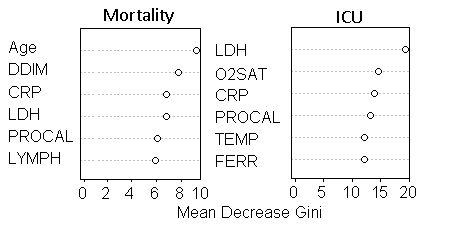
Results: A total of 635 patients were included in the analysis (age 60±11, 40.2% female). The top 6 mortality predictors were age, procalcitonin, C-creative protein, lactate dehydrogenase, D-dimer and lymphocytes. The top 6 ICU admission predictors are procalcitonin, lactate dehydrogenase, C-creative protein, pulse oxygen saturation, temperature and ferritin. The best machine learning algorithms predicted mortality with 89% AUC and ICU admission with 79% AUC.
Conclusion: This study identifies key independent clinical parameters that predict ICU admission and mortality associated with COVID-19 infection. The predictive model is practical, readily enhanced and retrained using additional data. This approach has immediate translation and may prove useful for frontline physicians in clinical decision making under time-sensitive and resource-constrained environment.
Keywords: coronavirus 2 (SARS-CoV-2), pneumonia, artificial intelligence, lung infection

 Global reach, higher impact
Global reach, higher impact